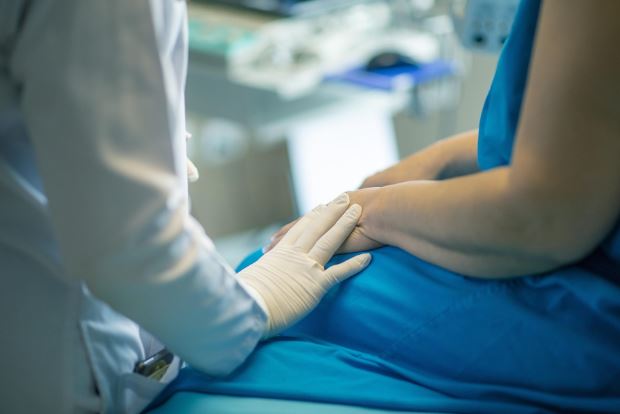
Medicare refers to a federal health insurance program developed to assist older U.S. citizens and people with disabilities in receiving the healthcare they need.
Sounds simple enough, but navigating the enrollment periods and knowing when you become eligible for Medicare can feel like solving a Rubik’s cube.
To help you match all the colors and make informed decisions about your healthcare coverage, we will break down the 3 enrollment periods for Medicare into pieces.
But first, let’s see what makes you eligible for Medicare.
Medicare Eligibility
Knowing when you become eligible for Medicare can not only help you plan your healthcare coverage but also save you from late enrollment penalties.
So, here are the conditions you need to fulfill to enroll in Medicare:
- You have to be a legal U.S. citizen for at least five years
- You must be at the age of 65
There are certain exceptions where you can be eligible even if you are under the age of 65.
These include:
- Having been diagnosed with end-stage renal disease (ESRD)
- Having been diagnosed with amyotrophic lateral sclerosis (ALC)
- Having been receiving the Social Security Disability Income (SSDI) benefits for at least 24 months
It’s also important to know that your income doesn’t affect your Medicare eligibility, but it will affect how much you will be paying for coverage.
Three Enrollment Periods for Medicare
To better understand what the 3 enrollment periods for Medicare are all about, we will take apart each one of them.
The Initial Enrollment Period (IEP)
The IEP starts three months before the month you turn 65 and ends three months after the month you turn 65.
Let’s say your 65th birthday is on July 15th. Your initial enrollment period would be on April 1st (3 months before your birth month), and it would include May, June, and July (your birth month)
and it would end on October 31st (3 months after your birth month).
That would include your 7-month window to apply for the initial enrollment period.
During this time, you can:
- Enroll in Medicare Part A (Hospital Insurance)
- Enroll in Medicare Part B (Medical Insurance)
- Choose to join (not mandatory at this point) a Medicare Advantage Plan (Part C) or a Medicare Prescription Drug Plan (Part D)
You would be enrolled in the IEP automatically only if you receive Social Security retirement benefits or Railroad retirement benefits for at least 4 months before you turn 65. In this case, you should receive a package in the mail 3 months before your 65th birthday containing your new Medicare card.
In any other instances, you would need to actively enroll in Medicare.
The Annual Enrollment Period (AEP)
Also known as the Annual Election Period, the AEP occurs annually and runs from October 15th to December 7th.
During this period, you can change your Medicare coverage options if you want to.
So, if you currently have only A and B Medicare parts, you can:
- Join a Medicare Advantage Plan (Part C) and opt for built-in drug coverage.
- Join the Medicare prescription plan (Part D) only.
If you currently have Original Medicare (Part A and/or Part B) and a stand-alone Medicare prescription drug plan (Part D), you can:
- Join a Medicare Advantage plan (Part C) and choose whether you want built-in drug coverage.
- Switch to another Medicare prescription drug plan.
- Opt out of prescription drug coverage completely.
If you currently have a Medicare Advantage plan (Part C) with built-in drug coverage, you can:
- Switch to another Medicare Advantage plan that can include drug coverage if you need it.
- Withdraw your Medicare Advantage plan and return to Original Medicare.
- Opt out of Medicare prescription drug coverage completely.
If you currently have a Medicare Advantage plan (Part C) and a stand-alone Medicare prescription drug plan (Part D), you can:
- Switch to another Medicare Advantage plan with or without built-in drug coverage.
- Switch to another Medicare prescription drug plan.
- Withdraw your Medicare Advantage plan and return to Original Medicare.
- Opt out of Medicare prescription drug coverage completely.
If you don’t make any changes to whatever your current Medicare plan is, your coverage will renew itself as is.
The Special Enrollment Period (SEP)
The SEP refers to a timeframe outside the Annual Enrollment Period when you can sign up for or change your health plan, provided you meet one of the following requirements:
- Losing health coverage (including Medicaid or Children’s Health Insurance Program (CHIP) coverage)
- Moving
- Getting married
- Having a baby
- Adopting a child
- Placing a child in foster care
- Getting divorced or legally separated and losing health insurance
- If someone on your Marketplace plan dies
- If you recently lost (or will soon lose) your Medicaid or CHIP coverage because your income is too high
- Becoming a U.S. citizen
In most cases, you will have 60 days to enroll in coverage, starting from the qualifying event date.
If you have any doubts about whether or not you qualify for the Special Enrollment Period, it might be best to consult a government source, such as HealthCare.gov.
Closing Thoughts
We hope we manage to simplify the three enrollment periods for Medicare and help you spend your golden years in peace, not worrying about your health plan.
Whether you’re approaching 65 or already enrolled, understanding these periods is crucial for making informed decisions about your healthcare coverage and avoiding potential penalties.